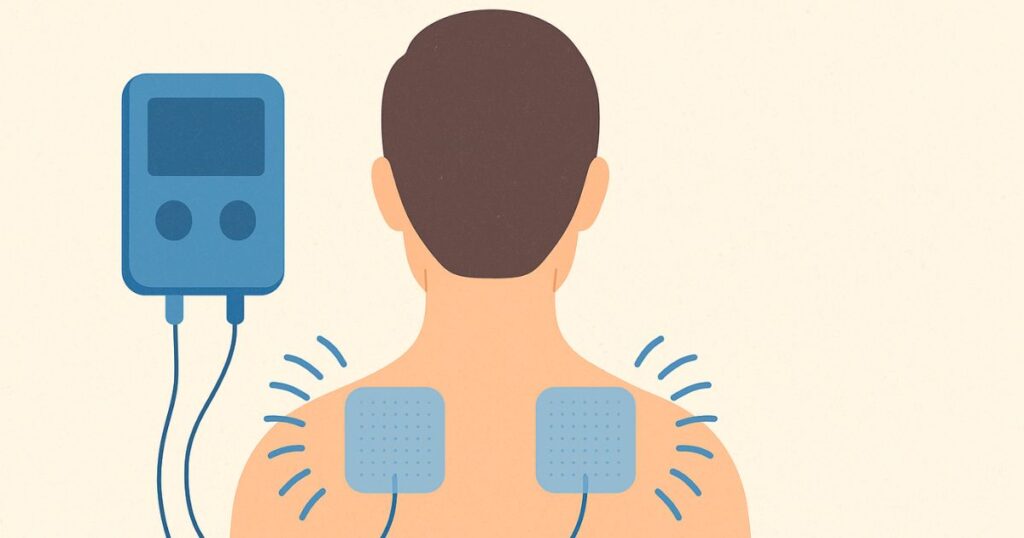
Transcutaneous electrical nerve stimulation (TENS) is a non-invasive technique commonly used for pain relief. Whether you’re navigating chronic pain, recovering from injury, or dealing with postoperative pain, a TENS unit may offer a pathway toward greater comfort and function—especially when integrated into a broader pain management strategy.
At Driftwood Recovery in Austin, Texas, we help individuals manage acute and chronic pain through personalized care, including access to supportive techniques like TENS therapy, when appropriate. Here’s what you should know about this widely used treatment.
What Is a TENS Unit?
A TENS unit is a small, battery powered device that sends electrical impulses through the skin using adhesive pads called TENS electrodes. These impulses stimulate nerves for pain control, without the use of medication or invasive procedures.
The term “transcutaneous” means “through the skin,” while “electrical nerve stimulation” refers to the process of sending current to the nervous system to influence how the body interprets pain signals.
Many TENS units are about the size of a deck of cards and can be purchased at a local pharmacy or through a pain specialist.
How TENS Works to Relieve Pain
Transcutaneous electrical nerve stimulation works by targeting nerve fibers responsible for transmitting pain. There are two primary ways it may help reduce pain:
- Spinal gating: High-frequency stimulation interferes with pain transmission at the spinal cord level.
- Central pain modulation: It promotes the release of natural endorphins, restoring central inhibition and reducing the perception of pain.
These effects are often described as temporary pain relief, but when used consistently and with adequate intensity, TENS treatment can support overall pain management goals.
When Is TENS Therapy Used?
TENS therapy is used to manage a variety of acute and chronic pain conditions, including:
- Chronic lower back pain
- Neck pain
- Chronic musculoskeletal pain
- Arthritis
- Fibromyalgia
- Multiple sclerosis
- Postoperative pain
It’s also frequently used by healthy human subjects and healthy volunteers in research settings to study pain responses and electrical nerve activity.
Types of TENS Treatment
There are two major types of TENS treatment, categorized by frequency:
High Frequency TENS (HF TENS)
- Uses stimulation over 50 Hz
- Typically produces strong but comfortable sensations
- Often used for immediate, short-term pain relief
Low Frequency TENS (LF TENS)
- Uses stimulation below 10 Hz
- Known to produce visible muscle contractions
- May support longer-term outcomes by engaging central inhibition
Selecting the right treatment intensity and stimulation intensity is crucial. In clinical use, the current should produce a strong but comfortable intensity without pain.
Evidence and Clinical Support
Studies—including randomized controlled trials, clinical trials, and systematic reviews—suggest that electrical nerve stimulation TENS can be helpful for many people with chronic pain.
Results vary based on electrode placement, duration, treatment session length, and underlying condition. The same frequency may not work for everyone, and exclusion criteria apply in cases of certain heart conditions or implanted devices.
Though it’s not a cure, TENS therapy can be a valuable component of a multimodal pain management plan—especially for individuals exploring options beyond medication.
Safety, Side Effects & Considerations
TENS therapy is generally well-tolerated. However, some users may experience skin irritation from repeated use of electrodes or adhesive pads. It’s important to:
- Follow device instructions and maintain clean skin
- Rotate electrode placement to avoid overuse of any single area
- Avoid using over broken skin or near the heart without clearance
Always consult a provider before beginning TENS therapy, especially if you have medical implants or a history of cardiac conditions.
What to Expect During a TENS Treatment Session
During a TENS treatment session, the unit is connected via lead wires to electrodes placed near the site of pain—sometimes even at acupuncture points. The device is activated, and you’ll feel tingling or pulsing—sometimes accompanied by mild muscle contractions.
Sessions typically last 15 to 30 minutes and may be used multiple times per day depending on your provider’s guidance.
Buying a TENS Unit
There are many TENS units on the market, with varying features:
- Adjustable treatment intensity
- Pre-set modes for neck pain, low back pain, and more
- Rechargeable vs. disposable batteries
- Number of channels and electrode pads supported
Check with your provider or local pharmacy to find a unit appropriate for your condition and lifestyle.
Is TENS Therapy Right for You?
Transcutaneous electrical nerve stimulation may benefit people looking to complement their existing pain relief plan with a drug-free option. Whether you’re recovering from acute pain or managing long term pain, TENS therapy may help reduce discomfort, increase function, and support your overall healing.
At Driftwood Recovery, we understand the emotional toll of chronic pain and help clients explore non-invasive options that fit their needs—always within the context of full-body, strengths-based care.
Frequently Asked Questions (FAQ)
Is transcutaneous electric nerve stimulation the same as TENS?
Yes. Transcutaneous electric nerve stimulation is simply a variation in phrasing for TENS, which stands for transcutaneous electrical nerve stimulation. Both refer to the same method of using electrical current and electrical pulses to stimulate nerves through the skin for pain control.
Can I use a TENS device at home without supervision?
Many people use a TENS device or TENS machine at home once they’ve received guidance from a medical provider. However, placement, frequency, and intensity settings are key to safe and effective use—especially for managing conditions like chronic low back pain or primary fibromyalgia.
Does transcutaneous electrical stimulation reduce pain intensity permanently?
TENS therapy is typically used to reduce pain intensity temporarily. While it can be part of a long-term pain management strategy, it does not cure underlying causes. Some users may experience a reduction in discomfort for hours after use, but lasting results depend on consistent application and overall health strategy.
Can using a TENS machine too often lead to tolerance?
Yes, in some cases, analgesic tolerance can develop, meaning the body becomes less responsive to the therapy over time. This is why alternating stimulation intensity, frequency, and treatment sessions is often recommended. Your provider may suggest rotating between low frequency and high frequency settings.
Is TENS therapy backed by scientific research?
Yes. There are many high quality studies, including randomized controlled trials, evaluating the effects of transcutaneous electrical stimulation on conditions like rheumatoid arthritis, chronic low back pain, and primary fibromyalgia. While individual results vary, research supports TENS as a safe and generally effective option for certain types of chronic pain.
Can TENS therapy be used for autoimmune conditions like rheumatoid arthritis?
TENS may help manage discomfort associated with rheumatoid arthritis, particularly during flare-ups. While it does not address the autoimmune cause, the electrical pulses can reduce perceived pain and help maintain mobility. Always check with your rheumatologist before integrating TENS into your routine.
Disclaimer
This blog is for informational purposes only and does not constitute medical advice. Please consult a qualified provider before starting any electrical stimulation or TENS therapy.
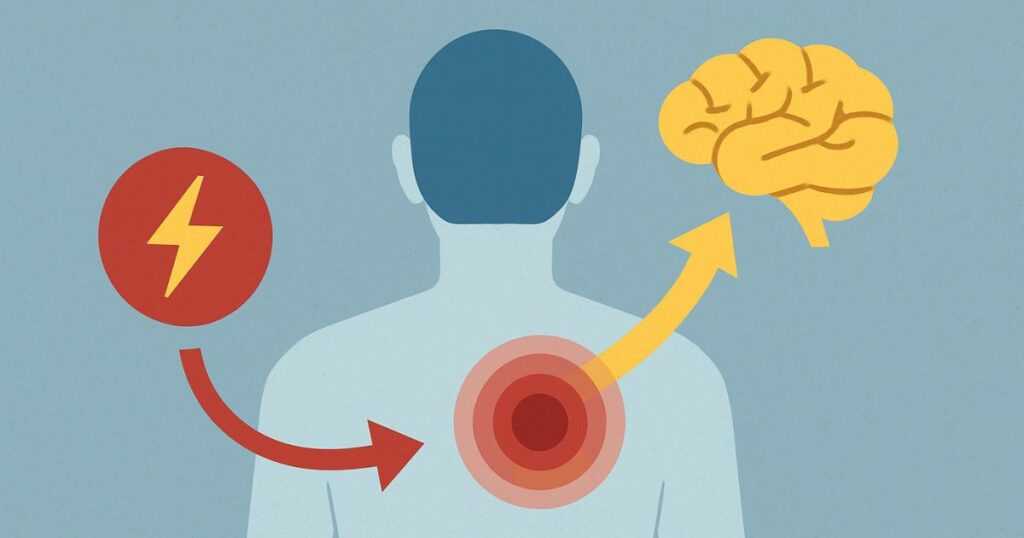
Central sensitization syndrome (CSS) is a term used to describe a group of conditions in which the central nervous system becomes hypersensitive—amplifying pain signals and creating symptoms that often go far beyond what traditional imaging or lab tests can detect.
For individuals living with chronic pain, this can be a frustrating and isolating experience. But gaining clarity around central sensitization is an important first step toward better pain management and improved quality of life.
At Driftwood Recovery in Austin, Texas, we offer compassionate, evidence-informed care for people navigating conditions like central sensitization syndrome, chronic fatigue, and medically unexplained pain. Our integrative approach helps clients not only manage symptoms but also rebuild trust in their bodies and develop a recovery lifestyle rooted in purpose and connection.
What Is Central Sensitization?
The process called central sensitization refers to changes within the central nervous system—particularly the spinal cord and brain—that increase responsiveness to pain. Over time, the sensory pathways become overly reactive, meaning that people may experience pain from stimuli that wouldn’t normally hurt, or feel intense pain that far exceeds the actual source.
This heightened pain response is known as pain sensitization, and it’s often accompanied by other symptoms such as fatigue, brain fog, sleep disturbances, and emotional distress.
Common Symptoms of Central Sensitization Syndrome
Although every individual’s experience varies, people with CSS often report:
- Chronic widespread pain, muscle tension, or tenderness
- Cognitive issues like cognitive difficulties or trouble focusing
- Emotional dysregulation, including anxiety and depression
- Medically unexplained symptoms that don’t respond to conventional treatment
- Hypersensitivity to light, noise, or temperature
- Lower pain tolerance and prolonged pain after injury
These symptoms suggest involvement of central neural plasticity, where the nervous system becomes stuck in a heightened state of reactivity.
How Pain Is Processed: Types and Sensitivities
The human body processes pain through a combination of sensory inputs and brain responses. When dealing with central sensitization, it’s important to understand how the body reacts to painful stimuli—and how those reactions can shift over time.
There are several types of pain that may be present in central sensitivity syndromes, including:
- Nociceptive pain: caused by tissue damage or inflammation, often related to injury or surgery.
- Neuropathic pain: resulting from nerve damage, often described as burning, tingling, or electric-like sensations.
- Pain hypersensitivity: a hallmark of central sensitization where even mild stimuli cause significant discomfort.
For individuals struggling with long-term symptoms, identifying central sensitivity syndromes is crucial. Interventions like physical therapy can play a major role in retraining the nervous system, reducing sensitivity, and improving function without relying solely on medication.
Conditions Linked to Central Sensitization
CSS overlaps with a number of chronic pain conditions, many of which are classified under central sensitivity syndromes. These may include:
- Irritable bowel syndrome
- Chronic fatigue syndrome
- Chronic pelvic pain
- Interstitial cystitis
- Chronic low back pain
- Chronic musculoskeletal pain
- Knee osteoarthritis
- Rheumatoid arthritis
- Neck pain
Often, these conditions fall under what are known as overlapping chronic pain conditions or overlapping disorders, making diagnosis and treatment especially challenging.
Diagnosing Central Sensitization Syndrome
There is no single test that confirms central sensitization, but tools like the central sensitization inventory and diagnostic criteria help clinicians evaluate a person’s symptom profile. A thorough physical examination, review of physical symptoms, and medical history are essential.
In clinical research, studies from journals like J Pain (Journal of Pain) and General Internal Medicine focus on establishing clinically significant values to better understand how CSS presents in chronic pain patients and how it differs from other prevalent pain conditions.
Risk Factors and Root Causes
Several risk factors contribute to the development of CSS, including:
- A history of acute pain that transitions into chronic symptoms
- Ongoing psychological stress and trauma
- Sleep disorders, psychosocial factors, or emotional overwhelm
- Genetic predisposition and relevant financial relationships (e.g., access to care or medication)
Many individuals with CSS report years of unexplained pain and failed treatments before finally receiving an appropriate diagnosis.
Treatment Options for Managing Central Sensitization
While there is no single cure, many strategies can help reduce symptoms and improve daily function. At Driftwood Recovery, our approach to managing chronic pain includes a variety of therapies that focus on both the body and mind:
- Cognitive behavior therapy (CBT) to reframe pain-related thoughts
- Pain neuroscience education and patient education to demystify symptoms
- Physical and occupational therapy to support mobility and desensitization
- Nonsteroidal anti inflammatory drugs, when appropriate, for symptom relief
- Holistic support for stress, sleep, and emotional regulation
Informed by systematic review and clinical experience with outpatient chronic pain samples, our team emphasizes collaborative care, ongoing education, and lifestyle interventions that address both physical and emotional healing.
Supporting Chronic Pain Patients Through Community and Care
Chronic pain is more than just a physical issue. It affects relationships, identity, and the ability to engage in life fully. That’s why at Driftwood Recovery, we treat people—not just symptoms.
Our approach to conditions like central sensitization syndrome is grounded in:
- Clinical practice that integrates mind-body therapies
- Therapeutic environments that promote community and accountability
- Tools for stress management and rebuilding a strengths-based identity
- Programs designed to lead patients into long-term recovery, not just short-term relief
Whether you’re living with centralized pain, nociplastic pain, or a mix of both, we believe healing begins when you’re truly seen, heard, and supported.
Final Thoughts
If you’re facing severe pain, widespread pain, or symptoms suggestive of central sensitization—and traditional medicine hasn’t provided answers—you’re not alone. Conditions like central sensitization syndrome are real, and with the right tools, they can be understood and managed.
Learn more about how our integrative approach supports individuals with central nervous system sensitivity and related conditions here in Austin.
Professional athletes have an increased risk of experiencing substance use disorder (SUD) at some point in their lives. According to the International Journal of Environmental Research and Public Health, “Athletes drink and use drugs for several reported reasons; to socialize, self-medicate pain/anxiety, and help falling asleep [. . .] It is thought that athletes’ attitudes towards drugs are heavily influenced by the culture of sports.” Staff members at treatment facilities face unique challenges in treating professional athletes due to their public-facing careers and pressure to achieve specific goals. The dedicated care team at Driftwood Recovery works together to ensure professional athletes have the support and resources to successfully achieve sobriety and manage unique challenges in recovery.
Choosing Residential or Outpatient Services for Professional Athletes
People with public-facing careers, including professional athletes, must consider their public image, health needs, and personal preferences when choosing treatment programs. Healthcare workers provide essential guidance for individuals who need additional help navigating substance abuse treatment. Clinicians at Driftwood Recovery understand the importance of maintaining client confidentiality and educating clients to ensure they make informed decisions to support their immediate and long-term treatment goals. One of the most important first steps is choosing between residential and outpatient treatment services. The level of care will help clinicians determine the most appropriate treatment services to meet the client’s needs.
Professional athletes can choose from multiple levels of care, including:
- Residential treatment (RTC)
- Partial hospitalization program (PHP)
- Intensive outpatient program (IOP)
- Outpatient
- Community integration program (CIP)
- Continuing care
Professional athletes may find it challenging to step away from their careers long enough to engage in residential treatment programs. Due to the increased schedule flexibility, intensive outpatient care provides the best outcomes for some individuals. Clients can attend to career and personal responsibilities while receiving essential addiction recovery support. The experts at Driftwood Recovery offer IOP and CIP.
Professional Athletes Have an Increased Risk of SUD
Substance abuse is prevalent in sports. According to Substance Abuse and Rehabilitation, “Athletic life may lead to drug abuse for a number of reasons, including for performance enhancement, to self-treat otherwise untreated mental illness, and to deal with stressors, such as pressure to perform, injuries, physical pain, and retirement from sport.” Staff members at Driftwood Recovery have experience treating career athletes and understand the importance of acknowledging the impact of sports culture on substance abuse. Many resources are available to help professional athletes achieve and maintain long-term sobriety.
Intensive outpatient services focus on preparing clients to manage their condition successfully while returning to a workplace where they may encounter individuals actively abusing substances. Clinicians play a vital role in ensuring clients recognize the need for support and use the resources at their disposal to prevent relapse, including:
- Individual and group therapy
- Support groups
- Peer engagement and mentorships
- Crisis management strategies
Driftwood Recovery treats professional athletes using personalized care plans designed to accommodate their specific needs and preferences.
How Do Clinicians Provide a Whole-Person Approach to Treatment?
Clinicians play an important role in introducing clients to sober living and strategies for creating a healthier lifestyle. The first steps in providing clients with a whole-person approach to treatment include:
- Making a genuine connection with the clients and their families
- Doing a deep dive into the factors impacting client’s mental and physical health
- Using comprehensive assessments and screening tools to ensure an accurate diagnosis
Client families, loved ones, and even teammates may be an essential source of helpful information during the initial phase of treatment. The clinical team ensures clients feel heard, understood, and supported. Gaining insights from the people closest to clients provides essential guidance for the care team. Healthcare professionals are also responsible for anticipating and addressing potential issues people may encounter after treatment by creating comprehensive aftercare plans.
The Importance of Aftercare for Professional Athletes
Continuing care services have become increasingly vital to sustained recovery for many people with SUD. Staff members provide clients with continued support, reducing the risk of relapse by ensuring clients have a lifeline if they experience challenges or a crisis. Career athletes have a higher risk of being triggered at work and in their private lives due to the prevalence of drug and alcohol abuse within sports culture. Clinicians mitigate those risks by providing healthy social connections, therapeutic support, and referrals to local recovery resources.
Continuing care services may include the following:
- Self-help groups
- Nutritional support
- Sober companions
- Mentorships or sponsorships
- Alumni services
- Individual and group therapy
- Family therapy
Athletes work in a high-stress environment and may feel pressured to end treatment quickly. Aftercare services help clients lower stress and manage cravings or other symptoms of SUD after they complete IOP treatment. The continued services provide motivation, emotional support, and additional accountability.
Healthcare Professionals Continue to Support Clients During Aftercare
Professional athletes have an increased risk of relapse due to multiple factors, including the prevalence of substance abuse in sports, chronic stress, pressure to perform well, and the increased risk of chronic or acute injuries. Addiction recovery specialists and other staff members support athletes during every stage of recovery, including the transition to aftercare services.
Confidentiality is critical during aftercare support. Healthcare workers are legally obligated to keep client medical information private and secure. The clinicians at Driftwood Recovery follow HIPAA guidelines and strict policies on recording and sharing client information. Many clients are more likely to follow through with aftercare if they trust their care team.
Intensive outpatient programs are ideal for individuals living or working in environments where they may experience frequent triggers. The time spent at home or work between treatment sessions allows clients to practice the life skills and coping techniques they learn in rehabilitation. Professional athletes have a higher risk of being surrounded by individuals who actively abuse or enable the use of alcohol or drugs. In addition, the clinical team must consider how public responses may affect athletes and other celebrities struggling with SUD. The experts at Driftwood Recovery help clients achieve sobriety and manage their condition using tailored treatment plans. To learn more about how our care team supports professional athletes, contact us today at (512) 759-8330.
Do I Need to Learn Emotional Regulation to Achieve Recovery?
Emotional regulation is a skill we begin to learn as young children. It allows us to recognize our emotions and express them. We spend this time learning to use healthy outlets for our emotions instead of unhealthy ones. However, if someone has struggled with trauma, abuse, and other factors beyond their control, they may bury their emotions or struggle to express themselves. It’s important to remember that just because a person may struggle with regulating their emotions now doesn’t mean that they cannot learn to do so later. It is never too late to seek help.
That’s why emotional regulation is an essential skill for those working towards recovery from addiction and other mental health conditions. As a result, mental health care and treatment facilities such as Driftwood Recovery include emotional regulation as a part of treatment. Alongside other life skills, such as stress management and relapse prevention, emotional regulation can be one of the keys needed for a long and happy recovery.
Understanding what emotional regulation is can be a bit confusing to those who have never heard of it. Thankfully, anyone can get a grasp on it once it’s broken down to its base concepts.
What Is Emotional Regulation?
There are several aspects to emotional regulation. Firstly, a person must be able to recognize what emotions they are experiencing. Second, they must healthily manage these emotions. Third, they must be able to respond to these emotions in a socially acceptable way. This does not mean that a person must keep themselves from experiencing strong emotions. Instead, emotional regulation is a tool that allows someone to accurately understand how they feel and respond appropriately.
For example, if you feel angry, it is not acceptable to hit or yell at another person to feel better. Instead, you can direct your anger into a productive and healthy outlet, such as painting. Emotional regulation can help someone manage their emotions without relying on drugs or other substances to numb them. A person who is used to hiding emotions to survive a past abusive situation may use emotional regulation to help them regain their full spectrum of emotions. Emotional regulation is not just a skill used to help manage emotions. It is also a tool used to help people heal.
Is There Such a Thing as ‘Bad’ Emotions?
An important fact learned in emotional regulation training is that there are no “bad” emotions. Our emotions exist for a reason. Without them, we become emotionally stunted and struggle with basic human connections.
An example of this is anger. People typically believe that anger is a bad emotion that people should strive to never feel. However, anger is an important emotion. It alerts you to injustices done against you and others. Anger is an emotion that inspires people to right serious wrongs in society. However, anger when used in in an unhealthy way can harm yourself and others. With training and practice, people can learn how to utilize an emotion like anger productively.
Ignoring your emotions is not healthy. Yes, emotions such as sadness when we experience grief or shame when we have done wrong to another are not fun to experience. However, these emotions help us learn and grow. The purpose of emotional regulation is to allow us to understand why these emotions are important and express them. Emotional regulation, however, is not to be used to decide what emotions you are allowed to feel.
Learning Emotional Regulation at Driftwood Recovery
At Driftwood Recovery, clients don’t just enroll to recover from their conditions. It’s also a place where a client can learn how to be a healthier person overall. Holistic treatment is about giving attention to all parts of a person during treatment. As a result, care is taken to address and nurture the emotional needs of each individual. Emotional regulation is a skill that is flexible enough to be incorporated into most therapies. This allows clients to obtain this vital skill, no matter what treatment program they are enrolled in.
Perhaps the most common way a client will receive emotional regulation training is through psychotherapy. Through therapies like cognitive-behavioral therapy (CBT), clients can learn how to recognize and accept their emotions. Therapies such as art and therapeutic recreation are used to teach clients how to express their emotions productively. These also allow clients to learn hobbies and other positive outlets for particularly difficult emotions.
Trauma-focused therapy is also important for those who have difficulties with their emotions due to trauma. It’s common for those who lived through trauma to attempt to bottle up their emotions. If they don’t acknowledge that these emotions exist, then they can pretend the traumatic event never happened. These therapies focus on using emotional regulation to allow clients to feel safe enough to express their emotions. It also helps clients learn how to regain their full emotional spectrum and feel confident once more.
Of course, every client is different, which is why each client is assessed when enrolling. This allows the professionals on staff to create a unique and individualized treatment plan. Those wanting help regulating their emotions should be honest with their treatment providers. They are not here to judge; they are here to provide help. Once you learn how to accept that help, you may find yourself feeling hope once again.
Learning how to regulate your emotions healthily is an important life skill. Without this skill, emotions like sorrow and anger can overtake you. This regulation can lead to several conditions, including addiction, in an attempt to cope with them. However, emotional regulation is a skill that can be learned and practiced. At Driftwood Recovery in Driftwood and Austin, Texas, clients learn life skills such as emotional regulation before they finish treatment. By utilizing this skill, clients have a greater ability to deal with stress and difficulty. If you are struggling with your mental health as well as regulating your emotions, don’t wait to seek help. Reach out today by calling (512) 759-8330.
Individuals diagnosed with substance use disorder (SUD) have a higher risk of experiencing physical injury and trauma, including traumatic brain injury (TBI). The presence of TBI may impact a client’s emotional stability, physical health, cognition, moods, and behaviors. According to the Journal of Neurotrauma, research has shown “that drug or alcohol intoxication itself increases [the] probability of suffering a TBI in accidents or acts of violence.” Driftwood Recovery treats SUD and co-occurring conditions, including TBI, using integrative care. Clinicians often must develop tailored treatment plans to address symptoms and underlying issues related to both conditions. The care team uses multidepartment support while treating traumatic brain injury as a co-occurring condition.
What Clinicians Have the Capability of Treating Traumatic Brain Injury and Substance Abuse?
Individuals with a traumatic brain injury may experience a wide range of side effects and symptoms. The care team must include professionals capable of effectively treating co-occurring medical issues and recognizing potential complications before they affect the client’s recovery. Interdepartmental teamwork is a significant part of providing high-quality treatment at Driftwood Recovery. Mental health, medical, and addiction recovery specialists combine their skills to provide a whole-person approach to care.
The presence of a TBI diagnosis changes how the care team treats and monitors individuals with SUD. Clients may be treated and supervised by internal and external medical professionals capable of recognizing the symptoms and side effects of TBI, including:
- Nurses
- Neurologists
- Physiologists
- Psychotherapist
- Psychiatrists
Integrative care is essential for individuals with TBI. Mental health and addiction recovery experts at Driftwood Recovery may collaborate with outside professionals monitoring the client’s health. Treatments for both conditions are more effective when healthcare providers work together to provide comprehensive and consistent care. A team of individuals is often needed to monitor the progress of healing for brain trauma. Recovery from TBI can take anywhere from a few weeks to several months, depending on the severity of the injury and the side effects.
The Benefits of Integrative Outpatient Services
Clinicians use integrative care to ensure clients have access to a whole-person approach to treatment. Holistic services often result in better outcomes and reduce stress by providing practical support to individuals with SUD and co-occurring conditions. Integrative care also reduces strain on the facility and staff by ensuring a team of qualified personnel can help clients with more complicated conditions, including clients with TBI. Intensive outpatient programs (IOP) are helpful for individuals with significant co-occurring health issues.
Some benefits of integrative outpatient programs include:
- Increased family involvement in the treatment process
- Easier access to outside care providers and services
- A broader range of support services
- More flexible schedule to accommodate doctor appointments
Integrative care involves a larger team of experts in various fields. Therapists, nurses, physicians, case managers, and other team members work together to ensure clients access relevant treatments.
How Does Treating Traumatic Brain Injury Alongside SUD Decrease the Risk of Relapse?
First responders, professional athletes, veterans, and active military personnel are among the most likely to experience co-occurring TBI and SUD. Careers with a higher risk of TBI may also feature an increased social acceptance of drug or alcohol abuse. In addition, substance abuse increases the likelihood of an individual experiencing an accident leading to severe injury.
Early interventions and rehabilitation reduce the risk of future brain injury and relapse, improving outcomes for individuals with TBIs. The presence of a traumatic injury makes it more likely future TBI will have more severe and potentially deadly side effects. Decreasing the likelihood of relapse helps individuals avoid experiencing preventable medical emergencies.
Treating a person’s TBI alongside SUD does the following:
- Ensures the care team maintains the client’s safety and health
- Reduces maladaptive behaviors related to the TBI
- Improves emotional stability and focus on recovery
- Increases accountability for following recovery instructions for both conditions
A TBI may cause significant changes in a person’s thoughts and behaviors. Generally, these changes last briefly and have only a minor effect on the person’s quality of life. However, individuals with SUD may experience more profound shifts in temperament, mood, and behaviors due to the combined effects of SUD and TBI on the physical structures of the brain. Healthcare workers must consider these factors when tailoring treatment plans and providing support services.
The dedicated experts at Driftwood Recovery understand the importance of using a whole-person approach to treatment for individuals with complex co-occurring medical issues. Clinicians have extensive training and experience assisting clients with a wide range of dual diagnoses, including SUD and physical trauma.
Healthcare Providers Assist Clients in Maintaining Healthy Lifestyle Changes
Healthy lifestyle changes are critical during early recovery for clients with co-occurring TBI and SUD. Diet, exercise, sleep patterns, social interactions, and other aspects of daily life are altered to support healing and recovery. Staff at rehabilitation facilities must often find creative solutions for supporting the health and well-being of clients with various co-occurring conditions, including TBI. The management team provides training opportunities for clinicians and support staff to increase their skills, allowing them to provide more comprehensive care for individuals with complex health issues.
Individuals with substance use disorder (SUD) have an increased risk of experiencing a traumatic brain injury (TBI) due to accident or injury. Vehicle accidents are a leading cause of TBI, especially in individuals with alcohol use disorder (AUD). The compassionate experts at Driftwood Recovery have the necessary resources and training to help people recover from SUD while healing from TBI. The symptoms and side effects of TBI exist along a spectrum. Everyone reacts differently to traumatic brain injuries. The clinical team collaborates with clients to ensure they receive comprehensive care. To learn more about how our team helps people recover from SUD and co-occurring health issues, call our office today at (512) 759-8330.
Recovery Community: The Healing Power of Connection and Engagement
According to the Journal of Clinical Medicine, recovery capital typically encompasses five domains. The five domains of recovery capital include human, social, financial, cultural, and community capital. Each domain is important, but the social, cultural, and community domains of recovery capital highlight the significance of connection in recovery. Therefore, expanding your awareness of your recovery community can help you maintain recovery. Through a recovery community, you can find the healing that engagement in a community of supportive peers can offer.
At Driftwood Recovery, we believe engaging in a recovery community is vital to building a strong foundation for sustained recovery. In an active recovery community, you can find the compassion, support, and accountability you need to thrive. Thus, through an attachment approach to care, you have learned the value of connection and community for healing. With a recovery community in alumni, you can continue to learn from and be supported by the compassion, understanding, and guidance you and your peers find in each other.
However, you may still have questions about what an active recovery community looks like. How can you engage with your recovery community to get the most out of your recovery?
What Is a Recovery Community?
A recovery community gives you the opportunity to connect with others who have shared experiences. Through shared experiences, you and your peers can learn how to build strategies and maintain coping skills for sustained recovery. As the U.S. Department of Health and Human Services (HHS) states, recovery support found in a recovery community recognizes that treatment alone may not sustain recovery. Therefore, access to a recovery community can give you the whole person care you need to thrive in every part of your life.
Yet, what does a recovery community look like? Beyond a network of peers, what makes something a recovery community? A recovery community makes it easier for you to engage with and stay connected in your recovery with a wide range of services and resources. As noted in Alcohol Research: Current Reviews, the recovery support services you can find in a recovery community include:
- Recovery high schools (RHS): Educational support to stay in or return to school to complete your high school degree
- Collegiate recovery programs (CRPs): Educational support to stay in and complete your degree in college
- Recovery homes: Community-style residences designed to support community reintegration and maintain a sober lifestyle
- Sober social events: Designed to introduce you to ways to socialize in events and activities without substances
- Recovery coaches: Trained peers mentor newer recovery members through shared experiences and supportive services
- Offer psychological, social, emotional, spiritual, employment, and financial resources
- Weekly alumni meetings: Allows you to stay connected with other community members to support social well-being
- Recovery community centers (RCCs): Typically a peer-operated local resource designed to help you build recovery capital
- Advocacy training
- Social services, employment training, skills training, and educational agencies
- Mutual help or peer-support meetings
- Social activities for peers, family, and friends
- Community involvement: Engaging in and giving back to your community supports community integration and fosters a sense of purpose
- Volunteer work
- Hiking group
- Book club
Therefore, the different services and resources offered highlight a recovery community as a valuable source of connection and, thus, healing.
The Importance of a Recovery Community for SUD
Fostering connection and community are invaluable to well-being in general. Through community, you can find your sense of belonging and build resilience to life stressors through mutual support from others. Thus, a recovery community is important to every domain of wellness on your recovery journey. Some of the ways a recovery community can help you heal from substance use disorder (SUD) and other conditions include:
- Support relapse prevention
- Foster healthy connections
- Reduce isolation in recovery
- Decrease feelings of loneliness
- Empower choices that support a recovery life
- Support building accountability and motivation
Thus, understanding the principles of community engagement can showcase the value of a recovery community as a part of your recovery.
Understanding the Core Principles of Community Engagement
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), community engagement is the process of developing relationships that enable communities to work together to address health-related issues and promote well-being. Although community engagement can take many forms, the core principles that can be supported in a recovery community include:
- Transparency
- Trust
- Diversity
- Inclusion
- Collaboration
- Shared purpose
- Openness
- Learning
- Making a difference in the community
- Sustained engagement
Within the core principles of community engagement, you can find healing and reconciliation to support the development of meaningful and trusting relationships. Through relationships built on trust and meaning, you can support sustained recovery.
The Value of Giving Back for Sustained Recovery
A recovery community gives you the space and resources to give back to your recovery community and the community in which you live. The process of giving back through community engagement helps you find purpose and meaning for motivation to sustain recovery. Listed below are some of the ways giving back supports maintaining your recovery:
- Promotes belonging and purpose
- Builds self-esteem and self-worth
- Fosters connection with others
- Distracts from cravings or triggers
- Fosters gratitude, compassion, and empathy
- Promotes personal growth and responsibility
- Expands your perspective
The sense of fulfillment that comes with engagement in your recovery community puts the value of healing the whole of your parts at the center of sustained recovery.
Finding a Recovery Community at Driftwood Recovery
At Driftwood Recovery, we believe a strong and vibrant alumni program can support your reintegration into daily life and sustain recovery. A peer network rooted in building connections fosters a recovery community in which healing is a whole-person process. Thus, the power of community empowers you to find and build upon the strength, hope, encouragement, and accountability you need to overcome the challenges to thrive. As a result, we are committed to making resources and services like weekly meetings, milestone dinners, and peer mentorship accessible across every stage of recovery.
Difficulties with addiction often lead to conflicts that fracture your relationships. Addiction can leave you feeling lonely and isolated from others. Without a support system, sustaining recovery is more difficult. You lack those important supportive connections that cheer on your successes and uplift you through challenges. However, with a recovery community, you can find, repair, and learn how to maintain those meaningful connections. Moreover, a recovery community gives you access to support services and resources that can help you heal and reintegrate into your community. Therefore, at Driftwood Recovery, we are committed to providing a vibrant alumni program to find purpose in life and recovery. Call (512) 759-8330 to learn how you can engage in your recovery community.
One of the fundamental feelings a person must consistently have for mental wellness is safety and security. Without the ability to feel safe and secure, it’s nearly impossible to maintain mental wellness. For example, it’s difficult for those in treatment to progress if they are constantly afraid of physical and emotional harm. It’s especially important now to stress how safe modern mental health treatment is, as its media portrayals are often less than ideal or rely on outdated depictions for a cheap scare. Without this reassurance, people are less likely to seek the help they need.
That is why at treatment facilities like Driftwood Recovery, care is taken to make sure that safety and security are upheld for every client. As our understanding of mental health care grows, so too does our ability to provide a safe and supportive treatment environment. This philosophy can be found at any mental health care and addiction treatment facility, allowing clients everywhere to be assured of their safety and security.
However, it can be difficult for someone to trust a treatment facility, especially if they have experienced judgment or belittlement in the past. To allow healing to reach those in need, we must explain why the values of safety and security in treatment facilities are upheld so strictly.
Why Is Safety and Security So Important?
As mentioned before, a lot of our mental health hinges on our feelings of safety and security. When we experience events or live in environments that strip away these feelings, it can be difficult to relax. Perhaps the most well-known conditions resulting from a lack of safety and security are anxiety disorders. Some common examples include post-traumatic stress disorder (PTSD), generalized anxiety disorder (GAD), and obsessive-compulsive disorder (OCD). People who struggle with these anxiety disorders often turn to external means to relax or quiet their symptoms. Usually, it ends in a substance use disorder (SUD), which quickly leads to addiction.
The ability to feel safe directly factors into how effective the treatment will be for an individual. If a person cannot relax and rest properly, they may experience burnout and frustration. This greatly slows progress and can cause someone to quit treatment altogether. It’s especially true for those who are more private and don’t want the world to know they are in treatment. Without this trust, people are often afraid to seek treatment, which prolongs their pain. To reduce this likelihood, a great effort has been taken to educate the public about modern mental health treatment to put these common fears to rest.
Understanding Modern Mental Health Treatment
One reason why someone may refuse treatment is that they are afraid. Modern media typically portrays rehab and other treatment programs as something akin to prisons. Our nation’s history of mental health treatment is often used as a prop in horror movies to scare their audience. It is not unusual for someone to believe that enrolling in a treatment program means being trapped while being subjected to outdated practices and abuses.
The truth is that the standards of safety and security of modern treatment facilities are high. These facilities are regularly inspected and staffed by professionals to make sure each client is safe. Modern mental health treatment is scientifically backed and is subject to peer review. If a safer and more effective treatment is discovered, modern mental health care facilities will make that treatment standard as quickly as possible.
It’s now common for mental health care facilities to choose to build in green and out-of-the-way places. By taking their facilities away from foot traffic, clients can recover with an increased level of privacy. Mental health care facilities are not places where clients can expect to be gawked at. Each mental health care professional and treatment provider understands the importance of safety and security for their clients to promote healing. After all, without the trust between provider and client, healing cannot proceed at all.
The Driftwood Recovery Approach to Safety and Security
Safety and security are important to the staff at Driftwood Recovery. Each client who enters treatment deserves to feel safe and secure. That is why many professionals are on staff to make sure each client remains safe.
For example, with medical professionals on staff, clients don’t have to worry about being too far away from help during a medical emergency. Specialized treatment providers who understand chronic pain help those who struggle with them find relief. Even those who participate in therapeutic recreational activities such as rope courses can expect to be cared for by professionals. No matter the activity, clients can be assured that it will be safe.
Safety and security are especially valuable to clients who have a public presence. No matter who the person is, they still deserve to recover in a peaceful environment. To meet this need, the staff at Driftwood Recovery make sure that their clients are not bothered and maintain client privacy and confidentiality at all times. Clients have access to quiet places to rest and recharge, preventing treatment burnout and promoting relaxation.
It’s always okay to ask staff members about the safety and security policies at Driftwood Recovery. They will be more than happy to explain their policies to reassure you that you are truly safe. If, for any reason, you feel unsafe, you are encouraged to speak to a staff member right away. The staff members care about you and your recovery and will work hard to make sure you feel safe. By extending trust in professionals to help you, it allows you to open yourself up to treatment. With trust, time, and treatment, you can recover from anything.
Those who are recovering from mental health conditions and chronic pain require a safe and secure place to heal. Without this security, it can be difficult for those in treatment to focus, which prolongs the time it takes to recover. That’s why at Driftwood Recovery in Driftwood and Austin, Texas, safety and security are important values that every staff member uphold. Here, clients can recover without worry that their privacy will be infringed upon. Under the supervision of professionals, clients can receive the comprehensive and compassionate treatment needed to achieve recovery. If you or a loved one is struggling with their mental health, call Driftwood Recovery today at (512) 759-8330.
In the past, older adults were less likely to be diagnosed with substance use disorder (SUD). However, the “Baby Boomer” generation has an increased risk of experiencing SUD. According to Clinics in Geriatric Medicine, “The prevalence rates of substance use disorder (SUD) have remained high among this group as they age, and both the proportions and actual numbers of older adults needing treatment of SUD are expected to grow substantially.” The mental health and addiction recovery experts at Driftwood Recovery use evidence-based and alternative holistic therapies to help seniors with substance use disorder build a sober future.
Increased Risk of SUD in Older Adults
Many factors have contributed to the rise in SUD among adults over the age of 65. Individuals born between the mid-1940s and mid-1960s, often called the “Baby Boomer” generation, have a more relaxed view of drug and alcohol abuse compared to earlier generations. Less judgment surrounding substance abuse makes it more socially acceptable. According to Addiction and Health, “With an estimated prevalence of 4%, substance abuse amongst persons who are 65 years and older is increasing [. . .] Substance abuse is difficult to recognize in the older adults, but once identified, presents its own challenges as only 18% of substance abuse treatment programs are designed for this growing population.”
Alcohol use disorder (AUD) and prescription drug abuse are the two most common addiction issues experienced by older adults. Some of the known risk factors for developing SUD later in life include:
- Substance abuse in childhood or young adulthood
- Mental health disorders
- Age-related cognitive decline or physical health concerns
- Chronic emotional or physical pain
- Lack of social support, social isolation, or loneliness
- Family history of substance abuse
Healthcare providers offering substance abuse treatment must find creative ways to accommodate the needs of older adults. For example, an older adult may experience memory lapses or other issues impacting their ability to participate in treatment. Case managers, nurses, counselors, and other staff members collaborate with each other, clients, and families to identify any age-related or co-occurring health issues that may impact a person’s ability to participate in treatment.
Treatment for Seniors With Substance Use Disorder
Driftwood Recovery and other treatment facilities offering care to individuals over 65 have a responsibility to provide appropriate treatment for seniors living with SUD and dual diagnosis. Often, older adults have multiple health conditions and prescription medications they take daily to manage their symptoms. The presence of specific disorders and medications may affect treatment for substance abuse. For example, older adults with chronic pain and opioid use disorder (OUD) may need additional support services to manage their pain without the aid of opioids, painkillers, or other highly addictive drugs.
Clinicians use comprehensive assessments to determine what factors may impact a client’s treatment and how best to support their health. Every member of an older client’s care team should have personal experience or training related to treating older adults for SUD and mental health disorders.
Seniors With Substance Use Disorder Face Unique Challenges During Outpatient Treatment
Everyone has a unique recovery journey. The care team is responsible for ensuring their skills and services provide clients with the necessary services to meet their needs and personal goals. Driftwood Recovery provides staff members with the resources to improve their skills to meet the needs of various demographics, including seniors.
Some of the most common challenges older adults may encounter during treatment for SUD include:
- Fear of stigmas, judgment from loved ones, or ageism
- Transportation issues
- Misconceptions about healthcare and mental health services due to generational differences
- Memory problems and difficulty remembering medications, schedules, and other essential aspects of treatment
- Medication side effects causing physical or emotional symptoms and side effects
Clients in intensive outpatient programs (IOP) must balance treatment with family responsibilities. In some cases, older adults require a higher level of care during the initial stages of treatment to ensure they remain focused on their recovery and have access to the resources they need to attend treatment sessions.
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), “Caregivers and families need resources to help navigate initial identification, screening, assessment, and treatment options for older people who misuse substances or have SUDs.” Intensive outpatient programs offer additional structure and support. Many older adults with SUD benefit from the greater flexibility of IOP, allowing families to become more involved in their loved one’s recovery.
How Does Driftwood Recovery Help Seniors With Substance Use Disorder?
Driftwood Recovery treats adults of all ages and backgrounds. Clinicians have the training, experience, and skills to provide older adults with the support they need to achieve and maintain sobriety.
The addiction recovery and mental health experts at Driftwood Recovery provide older adults and their loved ones with the following:
- Family therapy and support services to ensure family members play an active role in their loved ones treatment
- Information about how their diagnosis and any co-occurring disorders may impact treatment and long-term recovery
- Community-based and other local resources for addressing barriers to treatment, including transportation
Age-related physical disorders and the effects of some prescription medications may alter how seniors react to treatment for SUD. Staff are responsible for monitoring older adults throughout their recovery. Driftwood Recovery understands the importance of providing integrative, whole-person care to older individuals. The care team can work with the client’s family doctor and other outside members of their care team to create a positive and consistent treatment experience.
Older adults have unique needs and may require additional accommodations during treatment for substance use disorder. Rehabilitation programs require clients to actively participate in treatment by taking part in individual and group therapy, support groups, and other recovery services. Older adults might find it more challenging to attend treatment or remain engaged. Older adults may encounter unexpected health issues younger clients do not experience. Clinicians and support staff play an essential role in ensuring older adults have access to the resources they need to attend treatment sessions and maintain sobriety. The care team provides clients with a tailored treatment plan and essential support services. To learn more about the dedicated team at Driftwood Recovery, call us today at (512) 759-8330.
Individuals recovering from mental health conditions and substance use disorder (SUD) may experience severe or persistent symptoms, including anxiety, cravings, and intrusive thoughts. Relapse prevention is an essential part of managing symptoms and side effects of SUD. Ensuring accountability for clients and providing relapse prevention generally does not involve repressing or avoiding the triggers of relapse. Instead, treatment focuses on providing clients with the tools to manage them successfully.
According to the Yale Journal of Biology and Medicine, “Clinical experience has shown that occasional thoughts of [relapse] need to be normalized in therapy.” Healthcare workers are vital in ensuring people remain accountable for their behaviors while providing compassionate care. Therapy and other services help clients better understand themselves. Staff at Driftwood Recovery normalize conversations about mental health to facilitate healing and increase accountability.
How Does Encouraging Accountability for Clients Improve Outpatient Treatment?
The goal of treatment is to provide clients with the resources and skills to reintegrate into the community and improve their quality of life. Intensive outpatient programs (IOPs) focus on helping clients gain self-confidence, self-awareness, and coping skills for managing their condition in everyday situations. People in IOPs spend time between treatment sessions at work, home, school, or other locations where they may encounter triggers or stressors. Holding clients accountable for their actions during treatment prompts them to make healthier choices at home.
3 Ways the Care Team Supports Client Accountability
Staff members at Driftwood Recovery support clients and hold them accountable for their recovery by providing motivation, inspiration, education, and guidance. People struggling with substance abuse and mental health disorders seek treatment because they have been unsuccessful in achieving their health goals on their own. Staff ensure clients have the support and resources to maintain sobriety and positive mental health during and after treatment. Below are three ways the care team at Driftwood Recovery supports client accountability and long-term recovery.
#1. Setting and Monitoring Achievable Recovery Goals: Specific objectives keep the care team and clients on the same page and moving forward in the treatment process. Healthcare professionals use their relationships with clients to help them create practical and achievable goals. Clients are held accountable for working toward those goals with the assistance of their care team and support system.
#2. Relapse Prevention Education and Strategies: Psychoeducation helps clients make connections between their thoughts, beliefs, and behaviors. Clinicians educate clients to ensure they understand the importance of making healthier lifestyle choices and being accountable for their actions.
#3. Providing Clients With the Tools to Achieve or Maintain Steady Employment: Staff members often help people develop essential skills to achieve or maintain steady employment. According to Addiction, “In addition to financial rewards, employment can provide many incentives for sustained recovery, including purpose and meaning, social support, structure and accountability, and a sense of accomplishment and pride.” Clients often benefit from the structure and accountability of workplace responsibilities and expectations of sobriety.
Accountability for Clients Reduces the Risk of Relapse
Relapse is not an inevitable part of recovery. However, many clients participating in IOP treatment at Driftwood Recovery have a history of relapse and valid concerns about how to avoid backsliding into maladaptive behaviors. Staff are responsible for helping clients learn new ways to manage their condition and reduce the risk of relapse. Relapse prevention strategies, skill development, and social support help clients maintain sobriety and build a healthy foundation for the future. According to Alcohol Research and Health, treatment “interventions include identifying specific high-risk situations for each client and enhancing the client’s skills for coping with those situations, increasing the client’s self-efficacy, eliminating myths regarding alcohol’s effects, managing lapses, and restructuring the client’s perceptions of the relapse process.”
Every person responds differently to interventions. Healthcare professionals must work with clients and their families to determine how to address accountability and prepare clients for long-term recovery. Clients often change how they think and act when they know their choices impact the people closest to them.
Driftwood Recovery Facilitates Accountability for Clients
The dedicated experts at Driftwood Recovery have created a nurturing and welcoming environment by ensuring staff have the resources and training to provide personalized care. Tailored treatment services make it easier for the care team to hold clients accountable and encourage them to make healthier choices.
Staff members maintain accountability by doing the following:
- Making personal connections and developing a deeper understanding of the client’s needs
- Ensuring clients understand how their actions may impact recovery
- Providing emotional and practical support
- Encouraging families to play an active role in their loved ones recovery
- Providing relatable and relevant information and education
Support groups and peer engagement are essential factors in maintaining accountability. Clinicians encourage clients to engage with peers and join support groups. Studies have shown that “[s]upport groups provide guidance through peer feedback, and group members generally require accountability from each other.” The more consistently staff hold clients accountable for their sobriety, the easier it will be for clients to avoid relying on maladaptive behaviors after they complete treatment and transition to aftercare.
Individuals recovering from substance abuse and mental health disorders may experience severe or persistent triggers, including cravings or intrusive thoughts. Professional treatment offers clients essential support and reduces the risk of relapse by holding people accountable for their choices. Evidence-based and complementary treatments provide people with support and the resources to cope with everyday stressors. Healthcare workers are responsible for ensuring clients receive the level of care and personalized services they need to heal and recover from substance abuse. Driftwood Recovery uses tailored treatment planning and comprehensive assessments to help clients have positive outcomes. To learn more about how teamwork within healthcare facilities supports client recovery and sobriety, call us today at (512) 759-8330.
According to “The Role of Telehealth in an Evolving Health Care Environment,” the use of telecommunication and information technology in the health care system has been explored since the 1920s. From envisioning treating patients over the radio to establishing a closed-circuit television link between medical locations in the late 50s and early 60s, telehealth has been valued as a tool for connection and healing in medicine. Since its infancy, telehealth has been rooted in lowering barriers to care for underserved communities. Therefore, understanding virtual support tools is valuable to the process of recovery and sustained recovery.
At Driftwood Recovery, we believe connection and engagement in the community are vital to maintaining recovery. Thus, using virtual support tools like our Driftwood Recovery app allows you to strengthen those connections. Recovery should never be jeopardized because of a lack of resources for care and support. You deserve the same opportunities to thrive and sustain your recovery, no matter your level of recovery capital. With virtual support tools, you can dismantle barriers and expand your recovery capital to sustain recovery.
Yet, you may still have questions about virtual support tools and their relationship to telehealth. How does telehealth empower access to care?
What Is Telehealth?
Terms like telemedicine, telehealth, and telecare are often used interchangeably but can also have different meanings. As the Federal Communication Commission (FCC) states, telehealth, telemedicine, and telecare typically encompass advances in information and communications technologies for care. Specifically, information and communication advances allow medical professionals and other healthcare providers to offer remote and interactive services to consumers, patients, clients, and caregivers. Yet, the distinction in terminology can be important for understanding what virtual support tools are used and how those virtual support tools are used.
Listed below are some of the ways telemedicine, telehealth, and telecare are defined:
- Telemedicine: The use of telecommunications technologies to deliver different kinds of medical, diagnostic, and treatment-related services
- Typically utilized by doctors to diagnose, treat, and support patients
- Diagnostic testing, progress monitoring, and access to specialists
- Typically utilized by doctors to diagnose, treat, and support patients
- Telehealth: Evolved from telemedicine; thus, it shares similarities but includes a wider variety of remote healthcare services
- Services can be provided by other health and care providers like nurses, pharmacists, and social workers
- Can assist with health education, mental health literacy, social support, and medication management
- Services can be provided by other health and care providers like nurses, pharmacists, and social workers
- Telecare: The term is more commonly used in Europe and typically refers to technology like virtual support tools that allow clients to remain safe and independent in their homes
- Health and fitness apps
- Exercise tracking tools
- Digital medication reminder systems
- Early warning and detection technologies
The different terms highlight the variety of virtual support tools in health care. Thus, expanding your knowledge of virtual support tools can help you understand their impact on various areas of care.
Types of Virtual Support Tools
Since the COVID-19 pandemic, there has been a rise in awareness of telehealth and virtual support tools. The understanding of telehealth during the pandemic focused on preventative care to maintain social distancing. However, advances have opened the door to official and unofficial psychological virtual support tools. The virtual support tools that were expanded upon during the pandemic include mental health support, video conferencing, and multiplayer gaming. Specifically, the virtual support tools found in mental health services have expanded to meet clients where they are. As noted by the Substance Abuse and Mental Health Services Administration (SAMHSA), virtual support tools or virtual recovery resources can include:
- Virtual recovery programs
- Offers a variety of online meetings, discussion groups, forums, and access to services
- 12-Step programs like Alcoholics Anonymous, Cocaine Anonymous, Marijuana Anonymous, and Narcotics Anonymous
- Offers a variety of online meetings, discussion groups, forums, and access to services
- Online mutual-help groups
- Offers online and other virtual support tools to support specific and often underserved groups
- Women’s only recovery communities
- Programs centered on religious and spiritual beliefs
- Culturally sensitive and responsive programs
- Education, research, services, and resources
- Native Americans, Latinx, Black Americans, and LGBTQI+
- Education, research, services, and resources
- Offers online and other virtual support tools to support specific and often underserved groups
Virtual support tools highlight the ways information and communication technologies can support well-being.
Benefits of Virtual Support Tools for SUD and Mental Wellness
The remote nature of telehealth opens the door to more accessible and convenient treatment options for a wider audience. Moreover, telehealth can be particularly beneficial to the needs and care for various disorders and conditions:
- Real-time remote progress monitoring
- Provide resources for rapid intervention and crisis management
- Access to therapy and self-help recovery groups
- Tools for behavioral skill-building
- Texting interventions for relapse prevention
Further, as previously mentioned, virtual support tools are not only valuable for preventive care, crisis management, and skill building. Virtual support tools also work to dismantle barriers that impede access to services and resources in recovery.
Dismantling Barriers to Sustained Recovery With Telehealth
As noted by SAMHSA, millions of Americans are impacted by substance use disorder (SUD) and severe mental illness (SMI). Yet, 47.7% of Americans have an unmet need for mental health services, and only 12.2% of people receive treatment for SUD. The lack of treatment for SUD and SMI often stems from health disparities and inequities. Thus, telehealth, in conjunction with other accessible formats, can dismantle barriers to treatment and recovery resources:
- Improve the quality of care
- Decrease cost of care
- Improve client experience
- Increase engagement
- Improved access to continuity of care
- Supports aftercare
- Reduces stigma
- Decreases geographical barriers
Telehealth can address and support the long-term needs of clients with diverse backgrounds.
Staying Connected: Fostering Sustained Recovery at Driftwood Recovery
Health equity is an invaluable part of treatment and supporting sustained recovery. Through virtual support tools, you are given access to a wide variety of services and other resources to meet your needs. Therefore, at Driftwood Recovery, we are committed to providing a full continuum of care to support your recovery. No matter where you are on your road to recovery, we make support accessible to you. With our virtual support tools, you can continue to thrive and lead the courageous life in recovery you deserve.
Connection and engagement are important parts of treatment and sustained recovery. However, various barriers to services and resources can impede your ability to maintain recovery. Whether you are in early recovery or have been in recovery for years, you can experience challenges with cravings, triggers, and recovery capital. Yet, access to telehealth gives you virtual support tools to help you on your recovery journey. With access to apps, texting interventions, and remote progress monitoring tools, you can stay connected to your sober community, continue to build coping skills, and find support for relapse prevention and crisis management. Therefore, at Driftwood Recovery, we are dedicated to providing an accessible recovery community with our Driftwood Recovery app. Call (512) 759-8330 today.

